As the name suggests, in vitro fertilization (IVF) is used to fertilize eggs and sperm in a laboratory environment to produce an embryo (s). An embryo or embryos are delivered to the woman’s uterus via her cervix to increase the chances of conception. Infertility treatments such as in vitro fertilization (IVF) have advanced substantially in recent years. It is now used by heterosexual and same-sex couples and by single women hoping to have a family.
IVF laboratory procedures
The whole spectrum of IVF laboratory operations in SCI IVF HOSPITAL includes the following methods:
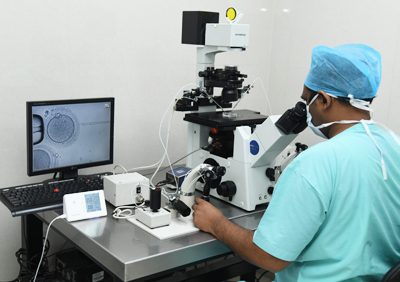
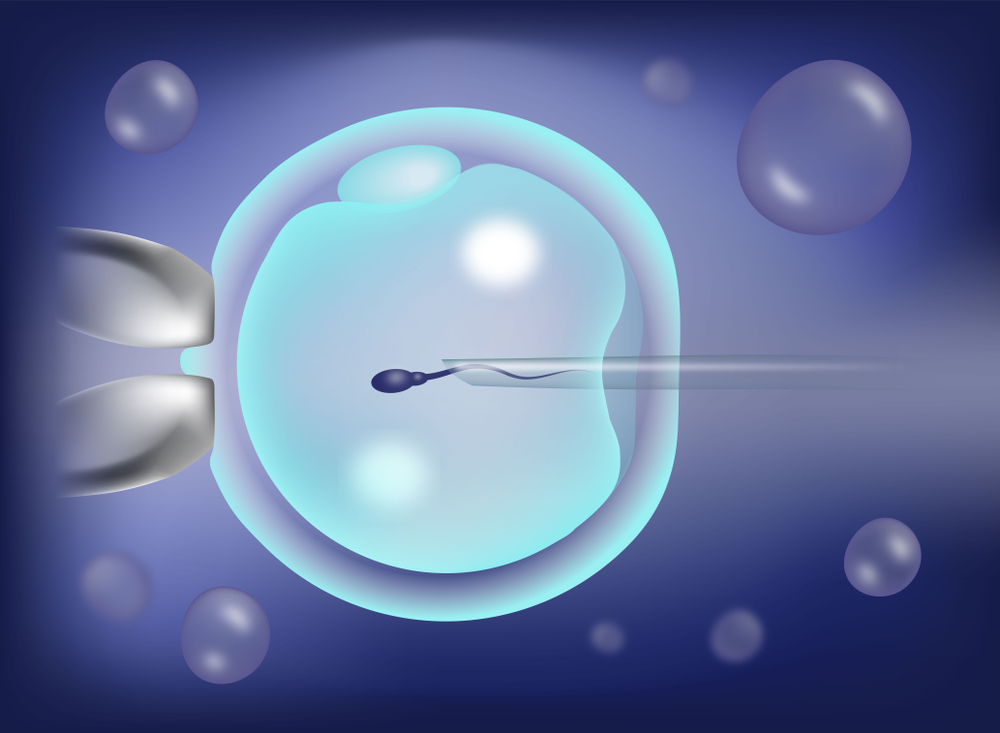
Fertilization with intracytoplasmic sperm injection (ICSI)
Using ICSI to fertilize eggs when sperm supply is low, sperm parameters are impaired, or other procedures have failed a thriving option. When the sperm count is very low or when there is no sperm in the ejaculate, IVF centre in Delhi NCR may effectively treat male infertility. Sperm may be harvested from the testicles or epididymis using a simple outpatient procedure in certain instances.
Assisted hatching
An embryo must break through the zona pellucida to implant in the uterus. “Hatching” refers to the embryo’s passage through the zona pellucida. Creating a small hole in the zona pellucida before transferring the embryo to the uterus may help in the hatching process. All embryos in an IVF protocol undergo assisted hatching before being delivered to the uterus.
Embryo freezing
The pair may be able to freeze (cryopreserve) embryos that are not transferred to the patient’s uterus for future use. After egg extraction, cryopreservation may be done either on the third or fifth day, depending on the embryo’s size, when it’s between 6 and 8 cells (the blastocyst stage). Cryopreservation is used for embryos that have the potential to become future pregnancies.
Genetic Screening for Chromosome Anomalies
The top IVF centre in Delhi is now providing a new method for assessing patient embryos and choosing those most likely to result in a pregnancy. At the blastocyst stage, a novel method called Trophectoderm Biopsy may remove numerous cells. Genetic and chromosomal abnormalities may be found in embryos as inherited genetic illnesses. The Genesis-24 test may be used to assess embryos from patients who have had several miscarriages or who are at risk for chromosomal abnormalities. To enhance the chances of having a healthy baby, it is necessary to do a chromosomal screening of the patient’s embryos and choose only healthy ones for transfer. Embryos may be transferred in the same IVF cycle using the Genesis-24 procedure.
Oocyte/ovarian tissue cryopreservation
Eggs and ovarian tissue are being frozen more often by IVF laboratories. Cryopreservation of ovarian tissue has resulted in just a few births, and it is definitely in its infancy. As a result of this, egg freezing is no longer considered an experimental procedure. For the following reasons, egg freezing may be a viable option:
- Women who have cancer and are set to receive chemotherapy may prevent them from producing eggs in the future.
- Women who are undergoing IVF aren’t comfortable having some or all of their embryos frozen.
- Women in their 30s who are postponing childbirth
Preimplantation genetic diagnosis (PGD)
IVF programme was the first in the area to introduce PGD. PGD entails the removal of a single cell from an eight-cell stage embryo. It is then tested for chromosomal and particular genetic abnormalities. Genetic screening of embryos is valuable for individuals with sex-linked illnesses or single-gene disorders like cystic fibrosis. These women may considerably lower the likelihood of their baby developing the condition by using IVF and embryo screening in tandem.
Conclusion
IVF is a costly procedure. Certain states compel health insurance providers to pay a portion or all of IVF cost in Delhi if specific requirements are satisfied. In contrast, many health insurance policies do not cover reproductive therapy at all.